Drug overdoses on rise in rural areas: http://bit.ly/VWvWag
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
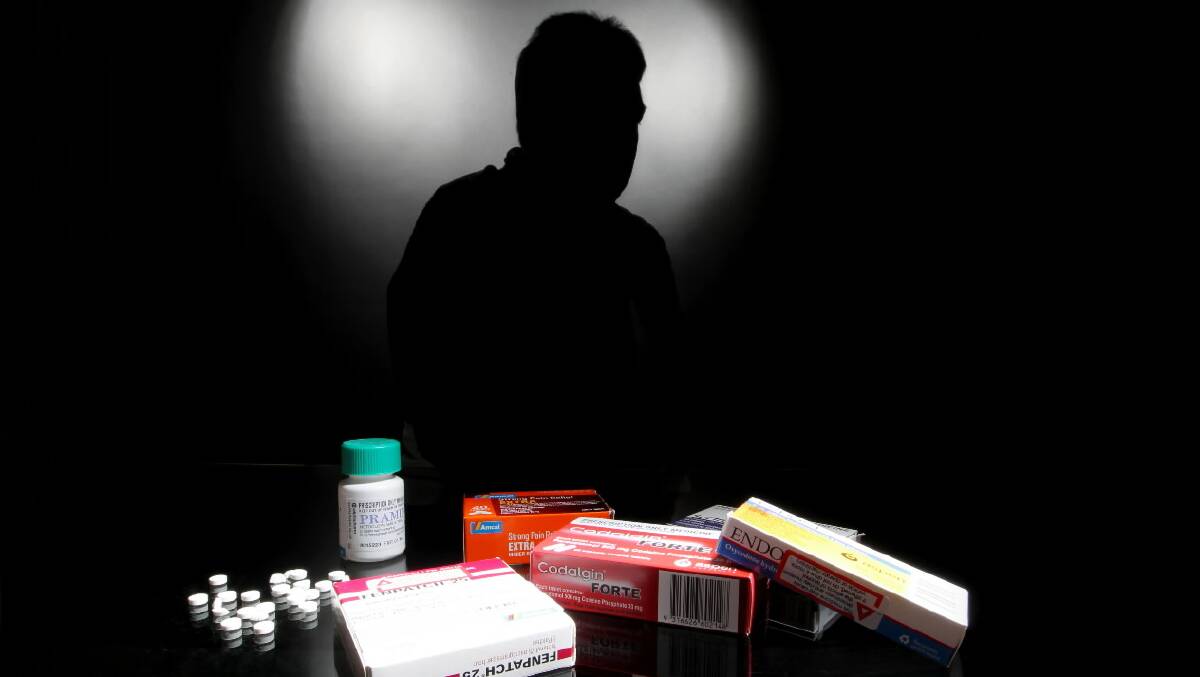
“I could not imagine a life without constant pain and drugs and was distressed that I had essentially become a bed-ridden drug addict.”
- Bob
IN A matter of a few months, Bob’s transformation was complete.
The optimistic, outgoing father-of-three with the “can-do” approach that led to multiple successes in his career had been reduced to a shadow of his former self.
Chronic pain had taken the joy out of his life and, in its darkest moments, left him questioning his will to live.
“I couldn’t see a future for myself,” the 56-year-old Wodonga single father said.
“I could not imagine a life without constant pain and drugs and was distressed that I had essentially become a bed-ridden drug addict.”
Bob could not have imagined that an opportunity to do a few weeks’ work in the idyllic South Australian setting of Kangaroo Island could end so badly.
But when an old back injury flared, he was left in agony and a long way from home.
In August last year, three days into his interstate assignment, Bob suffered what eventually turned out to be a rupture of a lumbar disc at the base of his spine.
“I had had back surgery 25 years earlier, but no serious lower back problems since,” he said.
Bob had to push on, in pain, until he could return to the Border in early September.
It took two weeks to see an orthopedic surgeon and get an MRI scan, which confirmed the rupture.
He was advised he needed the disc in his back replaced, with the earliest chance of the operation being just before Christmas.
In the four months between the injury and the operation, Bob was seeing his GP every week.
In a bid to manage his pain, he was on the maximum permitted doses of painkillers including Endone, Fentanyl, muscle relaxants and valium.
Initially, the drugs made him “disoriented, unable to think straight, and hesitant”, he says.
But as bad as the cure might have seemed, it wasn’t worse than the disease — Bob needed the medication just to get through each day.
Post operation, his recovery was slow and the drug regime continued.
In late February, unable to contemplate life continuing the same way, Bob sought an appointment with the Border’s only pain management specialist.
He got the earliest appointment he could, in late May.
The anxiety he had been dealing with had, by now, developed into severe depression.
He was given a course of Xanax by his GP, which he found had an immediate positive effect on his mental health. But government regulations in reaction to overprescription of the drug by less diligent GPs meant he could not get another course.
Bob started to see a psychologist.
“It helped settle me a little but the depression continued ... though suicidal thoughts lessened,” he said.
Finally May and his appointment with pain specialist Dr Brett Todhunter came around.
Bob was given the option of a spinal stimulation procedure, with the first available slot at the end of July.
His battle with pain raged on, as he waited for the procedure, hoping it might return some sense of normality to his life.
Despite another wait in hope that it would be the last, Bob said the care he received — particularly from his GP — was first rate.
“The level of care of my GP, the doctors and the nurses was absolutely second to none, as are the facilities,” he said.
“But specialists are very thin on the ground.”
One month on, he can finally say the pain has eased.
“I’d say it has gone from severe to light, or moderate,” he said.
“There are good days and bad days. But I probably have to accept the fact that I will be living with pain for the rest of my life.”
Managing that pain will be a continuing battle.
The next demon he must slay is the long and difficult withdrawal from the prescription drugs he has had to rely on heavily for nearly 12 months.
“Being on them (painkilling medicines) for a prolonged period is only good for one, obvious reason,” he said.
The downsides were the side effects, he says, and there were many. They included nausea, vomiting, constipation, anxiety and an inevitable dependence.
“My GP has been very clear about the gradual diminution of the doses,” he said.
“Going cold turkey is not an option.
“I have had some problems coming off them.”
Those problems have included feeling “shaky”, anxious, drowsy, nauseous and putting up with flu-like symptoms.
But Bob says the positive outlook he held before his injury has begun to return, and he is optimistic about his future, and hopeful it is free of the pain and drugs that came to dictate his life for the past year.
“I am an optimist but I have to accept the reality is that I will probably have to continue to cope with pain but to a much lesser extent,” he said.
“I know that I will probably have to do that for the rest of my life.
“But at least I have a life … there were many times when I couldn’t imagine I had one worth living.”
The Border Mail has agreed not to disclose the identity of the subject of this story.

